A Good Night’s Sleep for Better Health
A Good Night’s Sleep for Better Health


Why do you need sleep?
Sleep is as important to our health as healthy eating and exercise, but for up to 70 million people1 in the U.S., it’s often hard to come by. According to the Centers for Disease Control and Prevention (CDC), 14% of adults in the U.S. have trouble falling asleep and 17% have trouble staying asleep.2
For many, sleep disturbances can be so severe they’re considered a sleep disorder, such as obstructive sleep apnea (OSA). Although sleep apnea is common, which affects an estimated 30 million people, only 6 million receive a diagnosis.3
Even with a diagnosis, noncompliance with indicated treatment is a significant issue for many patients. Left untreated, OSA increases the risk for hypertension, heart disease, type-2 diabetes, liver problems, metabolic syndrome,4 and depression,5 and drives healthcare utilization and costs—to the tune of $94.9 billion a year.6
How does sleep affect chronic disease?
The relationship between sleep issues and chronic disease is well-documented. Research shows7 sleep problems are linked to an increased risk of diabetes, cardiovascular disease, obesity, and depression. Poor sleep is also associated with multimorbidity. A recent study8 in the journal PLOS Medicine found that individuals age 50 or above, who clocked less than 5 hours of sleep a night were 30% more likely to be diagnosed with multiple chronic diseases over time.
For patients suffering from chronic diseases such as congestive heart failure and type 2 diabetes, healthy sleep may be an enormously helpful, non-pharmaceutical way to improve quality of life, promote healing, and reduce health care costs.
Where can sleep studies be completed?
Diagnostic sleep tests, known as nocturnal polysomnography, can be performed in a facility or at home.
Home sleep tests can also be completed in the comfort of home if certain criteria are met. A home sleep test offers less intrusion without medical staff present and a better representation of an individual’s sleep in their environment. Turnaround times for results are also faster and the cost is lower.
What happens after a sleep study?
Even when patients are diagnosed with sleep apnea, a majority do not comply with their treatment, which is usually continuous positive airway pressure (CPAP) therapy. One study 9 found that more than 50% of patients had stopped using their CPAP within 1 year from the initiation of treatment.
CareCentrix offers a comprehensive sleep therapy and respiratory management program for health plans looking to better manage their chronic disease populations, reduce costs, and increase member satisfaction. The solution offers:
- Sleep diagnostic testing conducted in the home when clinically appropriate, thereby reducing costly facility testing and improving the member experience.
- Coordination of services to ensure members receive diagnostic testing in a timely manner and receive treatment faster if warranted.
- Monitoring and coaching from respiratory therapists and sleep medicine physicians to support adherence and utilization.
Payors that deploy the CareCentrix Sleep Management Program have seen:
- 80% of sleep diagnostic testing performed in the home
- 30% improvement in therapy adherence rates
- 20-30% annual savings
- 90% member satisfaction rate
Learn about the CareCentrix Home Sleep and Respiratory solution.
References
1 National Heart, Lung, and Blood Institute
2 Centers for Disease Control and Prevention: Sleep Difficulties in Adults: United States, 2020
3 American Medical Association
5 Journal of Sleep Medicine and Disorders
6 Journal of Clinical Sleep Medicine
7 Centers for Disease Control and Prevention: Sleep and Chronic Disease
Related Blog Posts

Sleep Health Literacy: The Key to Guiding Members from Diagnosis to Adherence
Just like diet and exercise, getting enough quality sleep is…
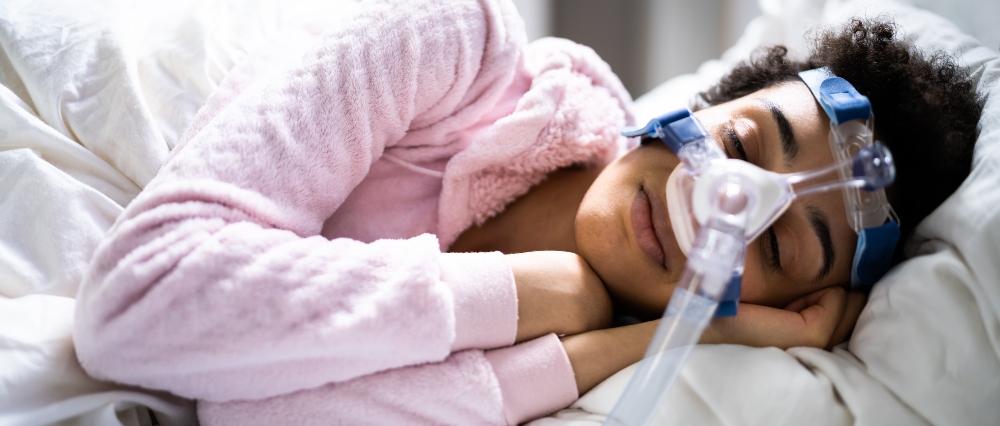
How Whole-Person Care Can Lower Cost of Care for CVD
Cardiovascular Disease (CVD) is a key area of focus for…
Why Culturally Competent Healthcare Is Vital To Whole-Person Care
I’ve worked in healthcare for nearly two decades, and as…
