The Hospital At Home
The Hospital At Home

Most Americans take it for granted that an acute-care hospital is available to them if they require surgery or become seriously ill. But this has been the case for only a relatively brief period of our history. Much routine medical care, and even some surgical care, was traditionally delivered in the patient’s home.
Hospital level of care
With the development of the modern hospital came the concept of “hospital level of care.” The concept assumed that there were treatments that could only be delivered in a hospital. These treatments initially were solely surgical procedures, but the scope of hospital level of care eventually expanded to include intravenous therapy, oxygen supplementation, and cardiac monitoring.
However, the benefits of hospital level of care came at a heavy price: hospital-acquired infections. Today, the CDC estimates that one in 25 patients (around 4%) develop some kind of hospital-acquired infection. These infections can be deadly. Even when they don’t kill, they are dangerous and expensive to treat.
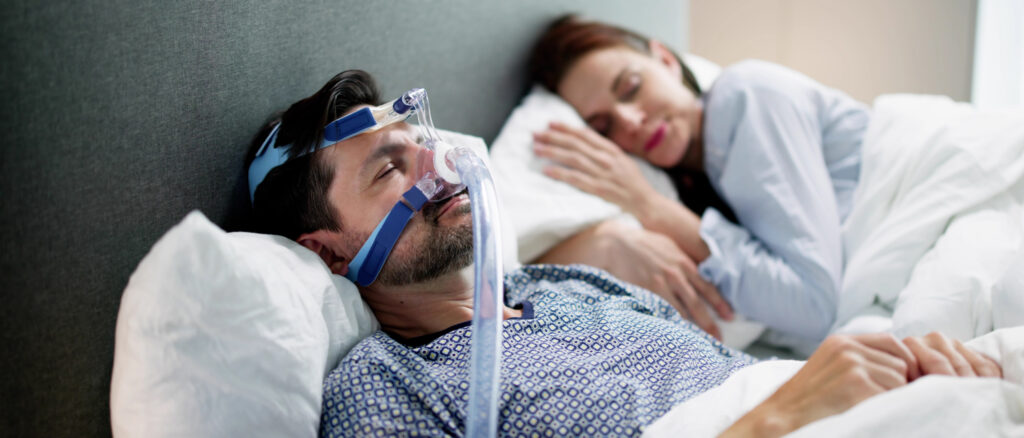
Hospitals have also become notorious for being places where it is nearly impossible to sleep due to uncomfortable bedding, round-the-clock hallway noise, and unappealing food. It is no surprise that a substantial effort has been underway in the world of medicine to move care of acute illnesses to settings more likely to enhance recovery, like patients’ own homes.
The hospital at home movement is born
In the mid-1990s, Johns Hopkins geriatrician Bruce Leff and colleagues pioneered a program to move acute care for some health problems from the hospital to the home. The first three conditions Dr. Leff’s team studied were community-acquired pneumonia, acute worsening of heart failure or chronic obstructive pulmonary disease, and soft-tissue infections. Their early results were encouraging.
Within ten years, the Hopkins team and other groups had generated a number of studies on the hospital at home concept, all showing essentially the same thing: treatment at home had lower mortality than did hospital treatment, treatment periods were shorter, and costs were dramatically lower. The responses from patients were overwhelmingly positive.
The Albuquerque experience
In 2008, Presbyterian Healthcare Services (PHS) of Albuquerque, New Mexico, launched a system-wide hospital at home program. In ten years, PHS has managed over 1,200 patients in their homes. The overwhelming majority are elderly: the average age of a PHS hospital at home patient was 77 years. Many patients were sent home for treatment from an emergency department. In fact, to be eligible for the program, a resident must live within 25 miles of a PHS emergency room. However, many patients enter into care at home from urgent care centers or even primary care offices. There are even referrals to the program made by home health agencies. A home assessment is critical to verify that the environment is suitable for hospital at home.
Barriers to the hospital at home
Despite some obvious advantages to the hospital at home concept, substantial barriers to widespread adoption remain. Most important among these is that the Medicare fee-for-service program does not cover hospital at home care. Another has been the reluctance of some physicians to become involved in the program. Most physicians today are trained to care for sick patients in the hospital. This is especially true of the relatively new class of physician known as hospitalists. Treatment at home represents a paradigm shift that many physicians are not ready to embrace. Finally, there is an economy of scale challenge. It turns out that a critical number of patients cared for at home are necessary to provide enough work for home hospital teams to function efficiently.
Overcoming the barriers
The problem of payment is gradually being solved. The recent 21st Century Cures Act promises to fund increasing numbers of programs to provide intravenous therapy and other treatments previously classified under hospital level of care. The problem of staffing is being ably managed by former emergency department nurses, who are especially adept at making rapid assessments and directing appropriate interventions in a timely fashion. The challenge of economies of scale could be met if more urban hospital systems were willing to adopt the hospital at home model.
Full circle
Dr. Leff jokes that “it’s still easier to get Chinese food delivered in New York City than to get oxygen delivered at home.” When the payment structure and other incentives become aligned properly, there is no reason to believe that home oxygen cannot be delivered in 20 minutes, without your neighbors getting menus stuck under their doors.
Related Blog Posts

Cancer Care Reimagined: Delivering Immunotherapy at Home
In the United States, the population is growing and living…

Closing the Gap: How Timely Delivery of Home Health Care Drives Better Outcomes
The High Stakes of Post-Hospital Care The transition from hospital…

Sleep Disorders: The Silent Epidemic Costing $94B Annually
Just like eating healthy, drinking enough water, and exercising, we…