My Personal Journey with Obstructive Sleep Apnea
My Personal Journey with Obstructive Sleep Apnea


This year’s Sleep Awareness Week is different for me. It’s not just a reminder of the importance of getting enough sleep and managing sleep-related disorders like Obstructive Sleep Apnea (OSA), it’s a time for me to reflect on what it’s like to be a person with OSA. It took me too long to get treatment, and I hope others won’t make the same mistake.
I lived in denial for a long time. I suffered many of the classic symptoms of sleep apnea: I chalked up my tiredness to the stresses of work and raising a family and not having enough hours in the day. I didn’t just snore, I snored loud enough that my wife couldn’t sleep, and she noticed that I would sometimes stop breathing, which scared her. And I knew my genetics were stacked against me: my dad had it, and my cousins have it.
As a physician, I was well aware of the risks of untreated OSA. As its name implies, Obstructive Sleep Apnea is when the airway becomes blocked or obstructed during sleep, usually by relaxation of tissues in the throat, which causes pauses in breathing (apnea). This degrades the quality of sleep, since each time breathing stops, the person awakens. It’s pretty hard to get a good night’s sleep when you are waking up every few minutes. People who are overweight are at higher risk of having OSA, but it also happens in thin people. It’s a chronic condition that can lead to serious health problems, including high blood pressure, heart failure, type 2 diabetes, and stroke. There are also secondary dangers from sleep apnea. High on that list is car accidents. People with sleep apnea are five times more likely to fall asleep at the wheel.
But it wasn’t until 2016, when I became Chief Medical Officer at CareCentrix, that I decided to finally get help. It seemed hypocritical for me to talk with clients and potential clients about how great our CareCentrix OSA home testing and treatment programs are, and not get tested myself. The team running the CareCentrix sleep program taught me that in-home testing is pretty easy, and that the machines currently used for treatment are more effective and a lot quieter than they used to be. And I learned about iComply, the program where respiratory therapists at CareCentrix coach newly-diagnosed OSA patients through the challenges of getting used to the machine.
So, I went to my primary care doctor and got an order for a home sleep test. CareCentrix approved it within 24 hours. The test was a little uncomfortable, but only required wearing a watch-like device on my wrist and wearing a sensor belt on my chest. It took me a few minutes to put the equipment on, and I slept in my own bed. It was a lot better than being wired from stem to stern and sleeping in a sleep testing center while someone watched me. And by having the test at home, I saved a lot of money – facility-based tests can cost double or triple what a home test costs.
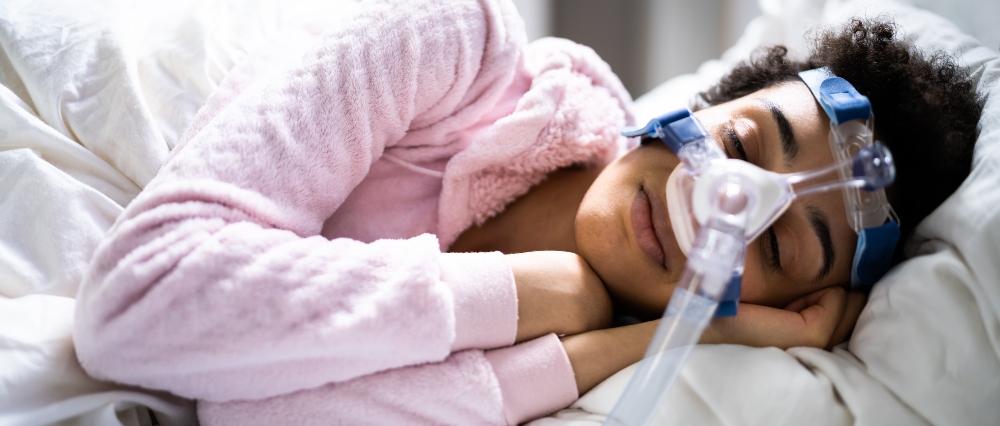
The test results were clear: I have severe OSA. The treatment is a Continuous Positive Airway Pressure (CPAP) machine. CPAPs work by blowing air into the nose and mouth, which keeps the airways open and prevents the person from having pauses in breathing. The machine I use every night is technically an APAP – an Adjustable Positive Airway Pressure device that has the ability to sense the need for more or less pressure and automatically adjust for it. The ability to sense and adjust the pressure saved me a night in a sleep lab – in the old days people with OSA had to go back for a second night of testing to make sure that the CPAP pressure was at the right level. The machine wirelessly sends information about my use of the machine to the manufacturer, who then shares that information with the respiratory therapists working in the iComply program.
I can also see a summary of my data by looking at the sleep report on the machine, or through an app on my smart phone. That has been helpful to me – it shows me how much time I’ve worn it, how many pauses in breathing per hour, and a lot more. This makes it easy for me to see when I am doing well, and when I need to get more sleep.
These days I feel better rested and more awake during the day. My wife is a lot happier too – I don’t snore, and she isn’t scared that I’ve stopped breathing. There are some challenges. It took me a few weeks to get used to sleeping with a plastic mask, head straps, and a flex hose, which make me look like a hazmat technician. I travel a lot for work, and carrying an extra bag is a hassle, but I’ve never had a problem at a security checkpoint.
Make this Sleep Awareness Week the one when you decide to do something to improve your sleep. If you or a loved one snores loudly, stops breathing when sleeping, or falls asleep during the day, don’t wait. Talk to your doctor about OSA and see if you qualify for a test.
If you want to measure your risk of OSA, there are short questionnaires you can use for free including the Berlin Questionnaire and the Epworth Sleepiness Scale.
Diagnosing and treating my OSA has made a real difference for me. I just wish I hadn’t waited so long to get help.
Related Blog Posts

Sleep Health Literacy: The Key to Guiding Members from Diagnosis to Adherence
Just like diet and exercise, getting enough quality sleep is…
A Good Night’s Sleep for Better Health
Why do you need sleep? Sleep is as important to…

Home Sleep Testing in the Age of COVID-19
The COVID-19 crisis caused major upheavals in all sectors of…
