The CareCentrix Model
CareCentrix empowers health at home by simplifying care coordination and home benefit management. We combine HomeFirst Analytics and personalized care to deliver the right services at the right time from hospital to home. CareCentrix enables seamless transitions of care, breaking down barriers to improve outcomes, lower total cost of care, deliver member and provider satisfaction, enhance quality of care, and guarantee savings.1
Solutions to Simplify Care Coordination and Home Benefit Management
A comprehensive solution to optimize DME benefit management in a timely and cost-effective manner.
A care coordination solution that connects members with home health services through a high-quality network.
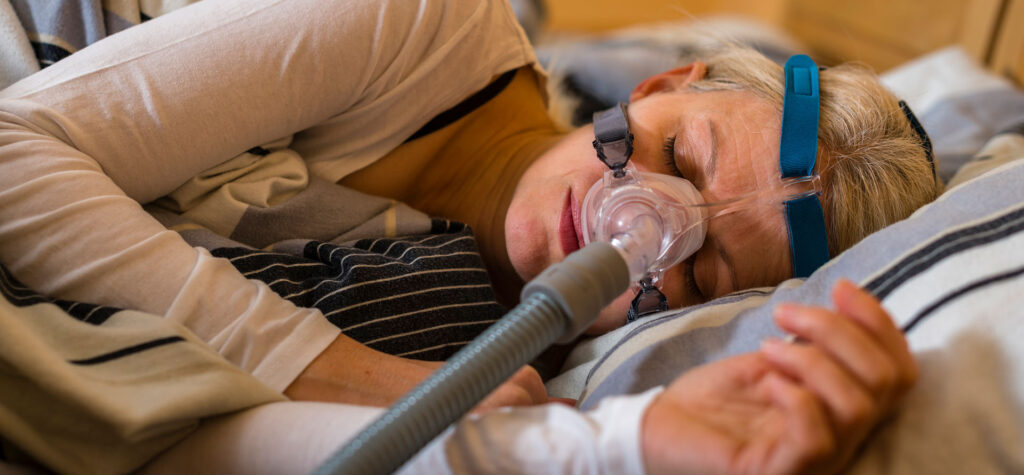
A holistic, cost-effective solution that supports sleep care in the right place, at the right time for members with sleep-disordered breathing.
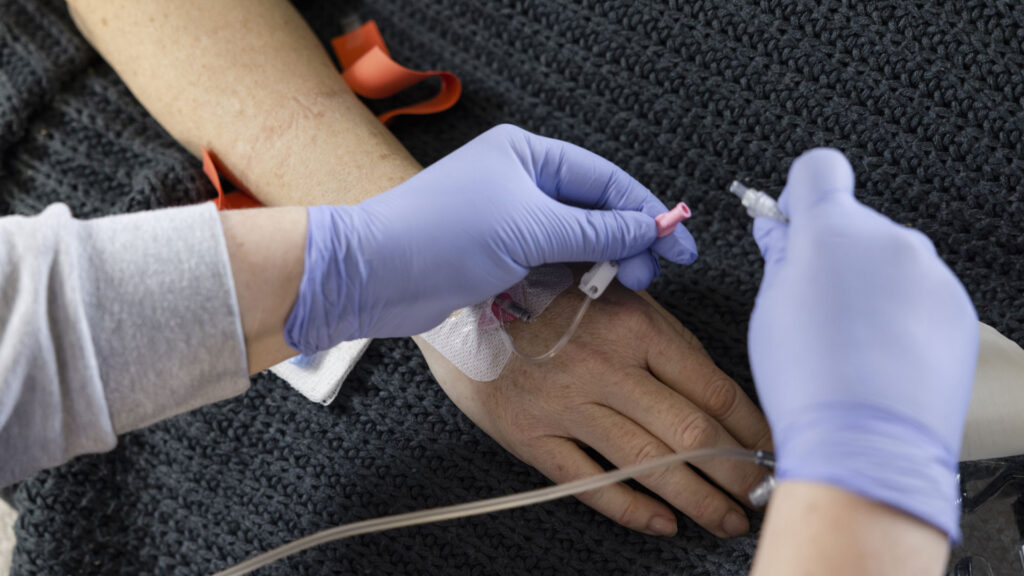
A flexible solution that optimizes access and supports coordination of infusion therapy for members at home.
A member-centric solution for immunotherapy infusions that shifts care from high-cost hospital settings to more efficient, member-friendly environments, such as the home.
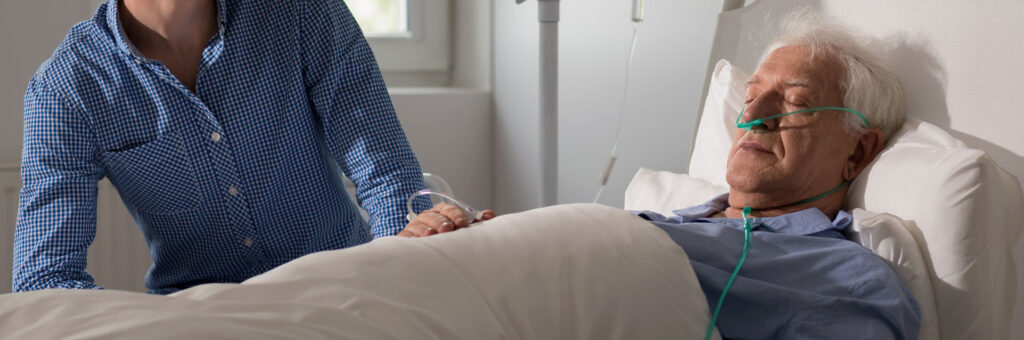
A personalized solution that helps improve quality of life and appropriately manages costs for seriously ill members.
A solution that eases the complexities of care transitions by identifying the most ideal pathways, optimizing lengths of stay, and supporting continuity of care.
A solution that enables seamless transitions to home, ensuring members receive necessary follow-up care—both clinical and non-clinical—to help reduce unnecessary hospital readmissions.

The Pace and Interest of Moving Care to the Home is Increasing
- 95% of people over the age of 55 prefer to receive services in the comfort of their home as they age2
- The average cost of a hospital readmission is 12.4% higher than the average cost of the original hospital admission.3
- 34% of home health services have reported delayed start of care4


Carecentrix empowers seamless, integrated home care
Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry’s standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged.

I am a heading
Here goes your text … Select any part of your text to access the formatting toolbar.

Method Matters
At CareCentrix, we believe empowering health at home is central to improving outcomes and delivering the right care. CareCentrix serves as the extension into the home, providing insights and solutions to enable successful care-at-home strategies.
Changing the way care is delivered begins with making the home more accessible and personalized.
- HomeFirst Analytics – proactively identify gaps in care, assess risks for readmissions, and connect members to the right support at the right time
- Personalized, Compassionate Care – engagement and support for members and caregivers throughout the journey
- High Quality Providers – network management that goes beyond just having adequate coverage to improve quality of care for more effective outcomes


The CareCentrix Savings Guarantee
CareCentrix solutions come with a financial guarantee that scales by membership growth. For nearly 30 years, our approach not only saves costs but also maintains high-quality care.



HomeFirst Analytics
+ Personalized Care at Home =
Guaranteed Savings & Satisfied Members
Whole Patient Care Coordination Solutions
Identify the best path of care and create discharge recommendations for members discharging to home, with an emphasis on home-first care delivery and preferred providers.
Coordinate and monitor the member’s transition home to reduce unnecessary hospital readmissions.
In-home palliative support for members with serious illness, and their caregivers.
In-home palliative support for members with serious illness, and their caregivers.
Network & Benefits Management Solutions
Facilitate access to a high-quality network of nursing, physical, speech, occupational therapy, medical social workers, and home health aides.
DME Navigator is a comprehensive solution that optimizes benefit management.
Provide flexible solutions to optimize access and coordination of infusion therapy for members at home.
Sleep testing and PAP therapy adherence support for members with sleep-disordered breathing.


















Lorem Ipsum is simply dummy text of the printing and typesetting industry. Lorem Ipsum has been the industry’s standard dummy text ever since the 1500s, when an unknown printer took a galley of type and scrambled it to make a type specimen book. It has survived not only five centuries, but also the leap into electronic typesetting, remaining essentially unchanged.
Lorem Ipsum
Lorem Ipsum