Improving Management of Infused Specialty Medications
Improving Management of Infused Specialty Medications

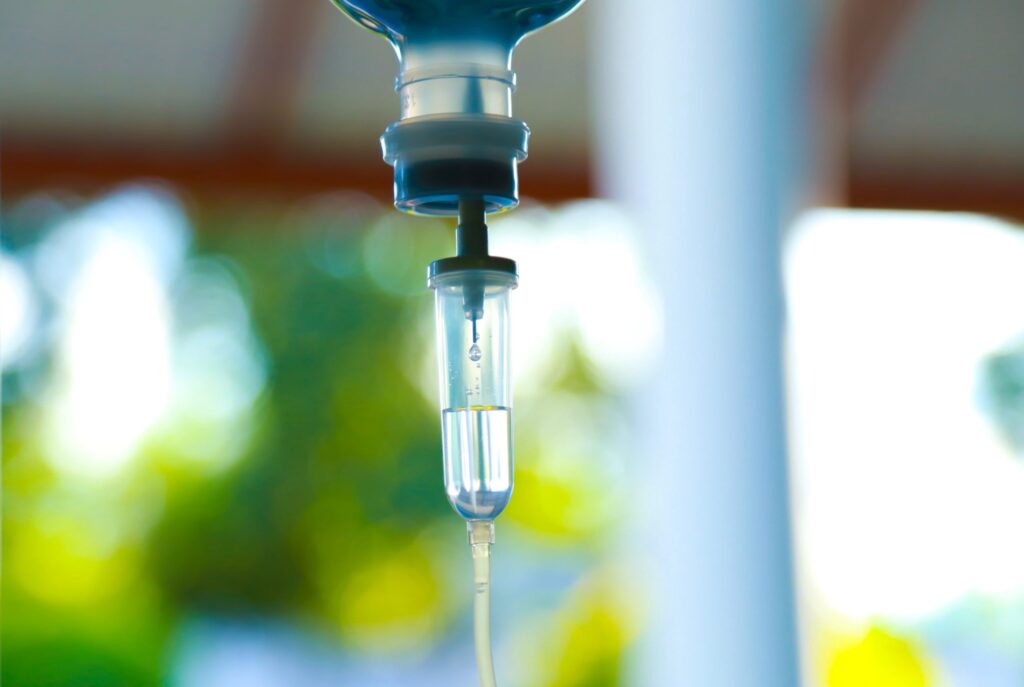
The increasing use and costs of infused specialty medications require new approaches that will not only decrease costs, but also improve outcomes and patient experience. Fortunately, there are solutions that go beyond the typical managed care approaches of “delay, deny and divert.”
Successful clinical management is possible through using four steps to improve management of infused specialty medications. First, use clinical rules to manage dose and preferred drugs. Second, focus on managing the site of care and move infusions out of hospital settings to home or ambulatory infusion suites. Third, choose the right partners – build a network of specialty pharmacy providers with clinical programs and scale. Fourth, actively manage clinical response to drugs – use clinical data to report response back to prescribers and assure that the patient is getting the optimal response to the medicine.
The good news is that many new infused specialty medications can be used to treat illnesses that previously lacked effective treatments, and usually with fewer side effects. The challenge is that the costs of these medications are staggering. From 2015-2020, the cost of infused specialty medications is anticipated to grow at an annual rate of over 11% to a cost of more than $20 billion/year. These costs are not sustainable, and require that these costly medications be used effectively and efficiently.
The 4 steps of an effective infused medication management strategy
Step One:
The first step to achieving more efficient use of infused specialty medications is to manage dose and preferred medications. Dose management is critical when differences in drug amounts can double the cost of an already expensive medication. The availability of bio-similar medications also makes it possible to reduce the costs of some infused specialty medications in the same way that generic medications and formulary management have been effective in reducing costs of medications managed under the pharmacy benefit.
Step two:
The second part of an effective infused medication management strategy is to manage the site of care. Infusing medications in the home or in ambulatory infusion suites (AIS) can cost 30-40% less than administering the same medication in a hospital-based infusion suite. Some health plans have already mandated home or AIS use for certain medications, and require clinicians to justify the additional expense of hospital-based. These approaches can generate significant cost savings, and make it easier and more convenient for patients to get their treatments.
Step three:
The third component of efficient specialty pharmacy management is to choose the right network. As in other aspects of care in the home or community, selecting the right providers can make a big difference in costs, quality, and outcomes. The home infusion market is currently fragmented, which both makes it difficult to choose a single partner to meet all needs, and also offers the opportunity to collaborate with smaller organizations that may be more innovative and willing to provide additional services.
CareCentrix is currently working with a payor partner to pilot administration of selected chemotherapy medications in the home setting. We interviewed many specialty pharmacies and found two smaller companies that had experience with these medications and were willing to invest in scaling their operations to provide more of these infusions in the home. Narrow networks for specific therapies to address therapeutic categories can be effective in improving clinical quality and achieving cost savings through directing volume to a smaller group of providers.
Step four:
The fourth and final part of an efficient and effective home infusion program is to provide feedback to clinicians prescribing the medications so that doses and intervals can be adjusted more frequently. Consider for example a patient with rheumatoid arthritis receiving infliximab (Remicade). The rheumatologist managing the patient may only see the patient every 2-3 months, and miss the opportunity to increase the dose to achieve better symptom control, or to reduce the time between infusions to ensure that the effects do not wear off between doses. Infusion nurses working with patients in the home can assess patient response to these medications and provide valuable and helpful feedback to guide change in dose and frequency.
Managing cost and improving care quality
It is the responsibility of all health plans to ensure efficient and effective use of infused specialty medications. Reviewing dose and preferred medications, assuring appropriate site of infusion, establishing high-performing networks, and providing clinical feedback, can more effectively manage cost and quality of care.
Related Blog Posts

Cancer Care Reimagined: Delivering Immunotherapy at Home
In the United States, the population is growing and living…

Closing the Gap: How Timely Delivery of Home Health Care Drives Better Outcomes
The High Stakes of Post-Hospital Care The transition from hospital…

Sleep Disorders: The Silent Epidemic Costing $94B Annually
Just like eating healthy, drinking enough water, and exercising, we…
4 Healthcare Trends that MA Plans Should Know in 2023
This year will be one marked by significant change and…

Delivering Care at the Community Level – A Common denominator at HLTH 2022
Each year, HLTH brings the entire healthcare industry together —…

The Future of Serious Illness Care: 3 Ways to Improve Your Strategy
With serious illness care being a highly uncoordinated part of…